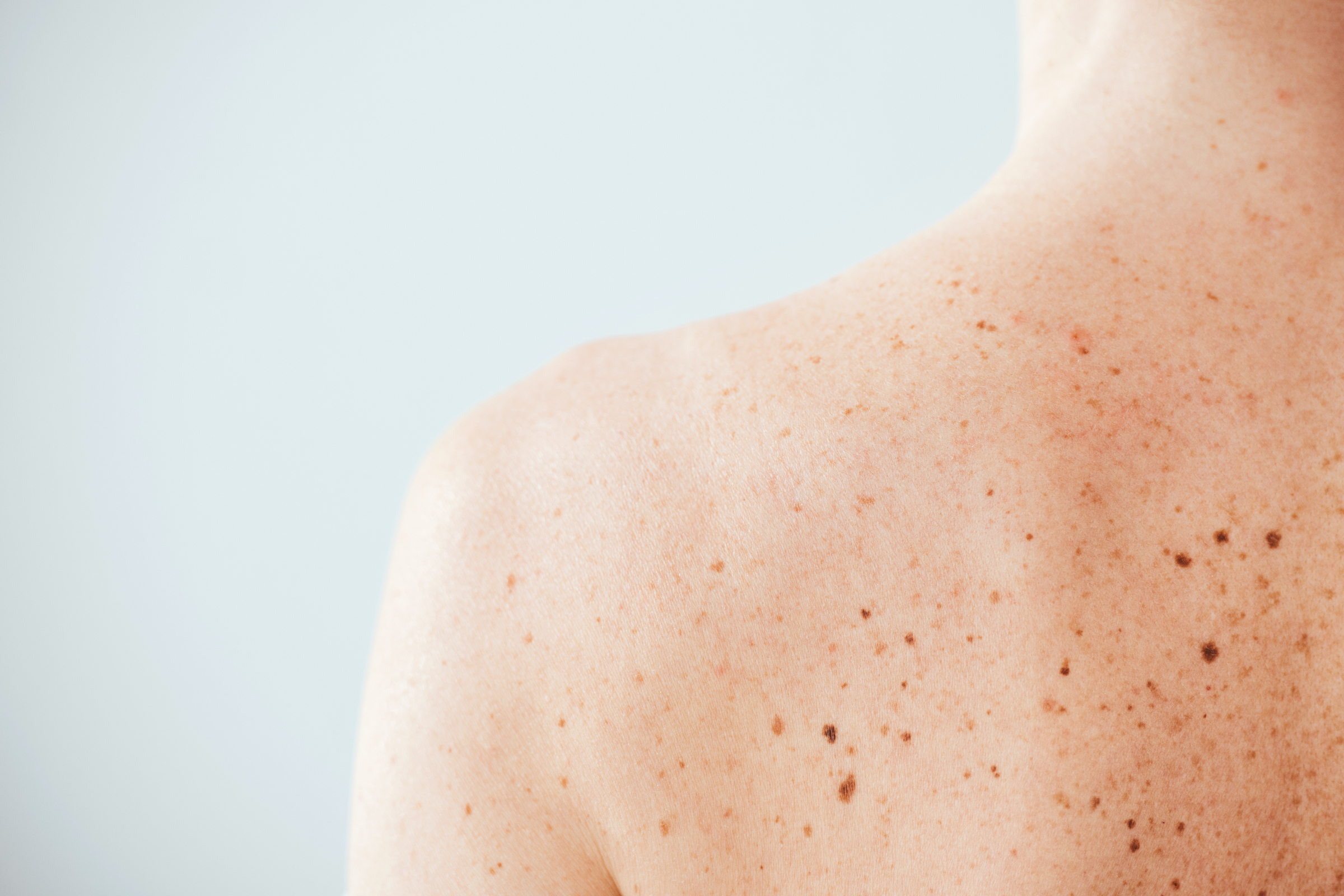
Diagnostic Assessment and Case ConclusionĪpproximately 1 month after the dermatologist visit, the patient presented to the emergency department for severe abdominal pain and vomiting. Additionally, he began to develop progressive fatigue and had 5 kg unintentional weight loss.įigure 1. They prescribed a high-potency steroid, but the patient’s itching continued to progress as did his upper abdominal pain. The patient saw a dermatologist several weeks later. Hence, in addition to prescribing a short course of 2.5% topical hydrocortisone cream, a dermatologist referral was made for follow-up. The provider caring for the patient in UC realized this was an atypical presentation, with a larger number of SK presenting so rapidly and with an unusual degree of pruritus. The SK were restricted to the posterior trunk and the remainder of his skin exam was within normal limits. His skin exam revealed numerous, diffuse SK distributed across his thoracic back (similar to the pattern seen in Figure 1). He was well appearing and had an unremarkable cardiopulmonary and abdominal exam. The patient had normal vital signs when he presented to UC. On review of symptoms, he was otherwise asymptomatic except for occasional postprandial abdominal pain, for which he used famotidine with minimal relief. He was sexually monogamous with his wife. He worked as a software engineer and denied alcohol and drug use. He denied any prominent family history of related conditions. 
The patient had taken some photographs with his smartphone which confirmed there were no lesions present on the back just 3 months earlier. The moles were restricted to his back and he had had no prior instances of skin lesions. Several weeks later, however, the pruritus became more severe and he began noticing the dark spots appearing on his back. His symptoms began with pruritus across the thoracic portion of his back, for which he had tried over-the-counter diphenhydramine with some initial relief. CLINICAL PRESENTATIONĪ 43-year-old man with no significant past medical history sought care at his local UC center due to itching and associated “moles” that had appeared across his upper back over the prior two months. 2 Given the seemingly innocuous nature of multiple moles, patients and clinicians alike may initially underappreciate the potential gravity of the phenomenon. It is nonspecific, however, and can also occur in benign conditions, such as pregnancy. 1 LTS can also occur in cases of hematologic malignancy. Lesar-Trélat Sign (LTS) is a paraneoplastic condition involving rapid appearance of multiple SK and is associated with a variety of solid organ malignancies, most commonly adenocarcinomas of the stomach, colon, and breast. Unfortunately, the patient died of complications of his cancer diagnosis several months after his UC presentation.Ĭonclusion: Awareness of the potential clinical significance of LTS and its association with occult malignancy may lead to earlier referral, cancer identification, and improved prognosis for afflicted patients. 
After computed tomography of his abdomen and esophagogastroduodenoscopy (EGD), he was diagnosed with metastatic gastric adenocarcinoma. His increasing abdominal pain eventually led him to present for care in the emergency department. He was prescribed hydrocortisone 2.5% cream and referred to a dermatologist.Ĭase resolution: Several weeks later,the patient saw a dermatologist who prescribed a higher-potency steroid. Physical exam: The patient’s skin exam revealed diffuse hyperpigmented ovoid lesions consistent with seborrheic keratoses (SK) restricted to his back. He also had some vague upper abdominal pain and unintentional weight loss. Given that the primary manifestation is a seemingly benign dermatologic issue, such patients may choose urgent care as their initial site of clinical evaluation.Ĭlinical presentation: A 43-year-old man with no significant past medical history presented to UC with complaints of itching and “moles” appearing across his back for the past 2 months. Introduction: Lesar-Trélat sign (LTS) is an infrequent paraneoplastic phenomenon associated with an array of malignancies. Key words: paraneoplastic syndrome, gastric cancer, seborrheic keratosis, case report ABSTRACT
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
